January 2022
Osteoporosis and Foot and Ankle Health
Osteoporosis is a bone disorder that causes the bones to become thin, brittle, and weak due to a lack of calcium and vitamin D. Although it is particularly common in women over 50, younger people and men can also develop osteoporosis. Since osteoporosis weakens the bones, it makes fractures more likely. Often, the first sign of osteoporosis is a broken bone in the foot. Symptoms of this include pain, redness, and swelling around the site of the fracture, and difficulty walking. A podiatrist can diagnose a broken foot bone through physical examination and X-rays. If you suspect that you may have broken a foot bone, or if you have been previously diagnosed with osteoporosis and want to learn more about preventing foot fractures, it is suggested that you consult with a podiatrist today.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact John Killough, DPM from Regional Foot Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Why the Ball of Your Foot Feels Like It Is on Fire
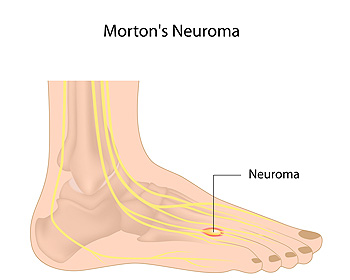
Morton’s neuroma occurs when the tissue surrounding a nerve in the toes thickens in response to the nerve becoming entrapped, or otherwise irritated. This usually occurs between the third and fourth toes, however, it can also occur between the second and third toes. Morton’s neuroma can cause a burning pain in the ball of the foot. People with this condition sometimes explain the pain they feel as walking on a pebble or having a bunched-up sock in the front of their shoe. The toes may also feel numb or tingling, and there may be difficulty walking. Wearing shoes that are too tight or that compress your toes may sometimes contribute to the formation of Morton’s neuroma. This can include ski boots and ballet slippers too. Other foot dysfunctions that squeeze or put pressure on the toes can be contributing factors, such as flat feet, bunions, hammertoes, and high arches. Certain repetitive sporting activities may also be responsible. If you ever experience any of the symptoms mentioned here, call a podiatrist. They will examine you and run diagnostics to rule out other possible conditions and create a treatment plan to relieve pain and treat the underlying thickened tissue and nerve compression.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact John Killough, DPM of Regional Foot Center. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Reminder: When Was the Last Time...?
Why Are My Toes Turning Blue?
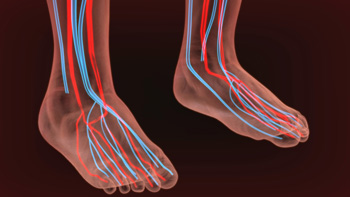
If you notice that your toes look bluish in color, you may have a condition known as peripheral cyanosis. The main causes are a lack of blood reaching the toes, and lack of oxygen in the blood that does reach the toes. Normally, when blood is properly oxygenated it turns bright red. When oxygen levels are low, the blood turns a burgundy, or more bluish, color. However, if the toes are not receiving enough blood, even though it is fully oxygenated, the result is still a bluish color in the toes, and other body parts as well. The main causes of decreased oxygen are a blockage that prevents blood from reaching the extremities, or lack of pressure sufficient to allow the blood to reach the extremities. A fatty buildup in the blood vessels, known as peripheral arterial disease (PAD) is a common factor in such blockages. If you notice that your toes appear to be bluish, it is suggested that you make an appointment with your podiatrist, who can offer a proper diagnosis and treatment options.
While poor circulation itself isn’t a condition; it is a symptom of another underlying health condition you may have. If you have any concerns with poor circulation in your feet contact John Killough, DPM of Regional Foot Center. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Peripheral artery disease (PAD) can potentially lead to poor circulation in the lower extremities. PAD is a condition that causes the blood vessels and arteries to narrow. In a linked condition called atherosclerosis, the arteries stiffen up due to a buildup of plaque in the arteries and blood vessels. These two conditions can cause a decrease in the amount of blood that flows to your extremities, therefore resulting in pain.
Symptoms
Some of the most common symptoms of poor circulation are:
- Numbness
- Tingling
- Throbbing or stinging pain in limbs
- Pain
- Muscle Cramps
Treatment for poor circulation often depends on the underlying condition that causes it. Methods for treatment may include insulin for diabetes, special exercise programs, surgery for varicose veins, or compression socks for swollen legs.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions, please feel free to contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Making Sense of Plantar Fasciitis
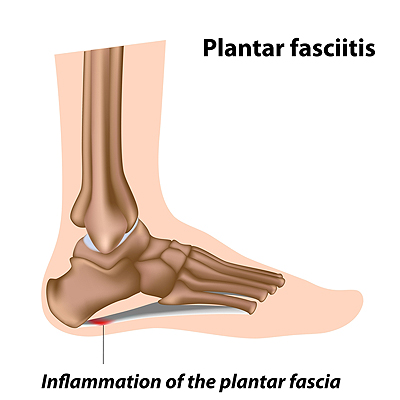
The fascia is a long, fibrous band of tissue that connects the ball of the foot with the heel bone. When that tissue becomes injured or damaged it can tear, and become inflamed and painful. This is a condition known as plantar fasciitis. There are many reasons why plantar fasciitis can occur, including wearing shoes that don’t provide adequate support, having a job that requires you to stand all day, and being obese, old, or very physically active. Certain structural anomalies, like high arches and flat feet, or alignment/gait issues can also contribute to plantar fasciitis developing. A telltale sign of plantar fasciitis is pain that is intense when you first wake up, and then gets gradually better as the day progresses. Since plantar fasciitis is the most common form of heel pain, podiatrists have a great deal of experience treating this condition. They may use rest, ice, physical therapy, night splints, and orthotics to treat it. If these protocols don’t yield optimum results, the podiatrist may use extracorporeal shock wave therapy to heal pain and boost the body’s natural healing process to repair the damaged plantar fascia. If you believe you may have plantar fasciitis, it is suggested that you see a podiatrist for an accurate diagnosis and expert treatment.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact John Killough, DPM from Regional Foot Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our offices located in Charleston and Effingham, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Plantar Fasciitis